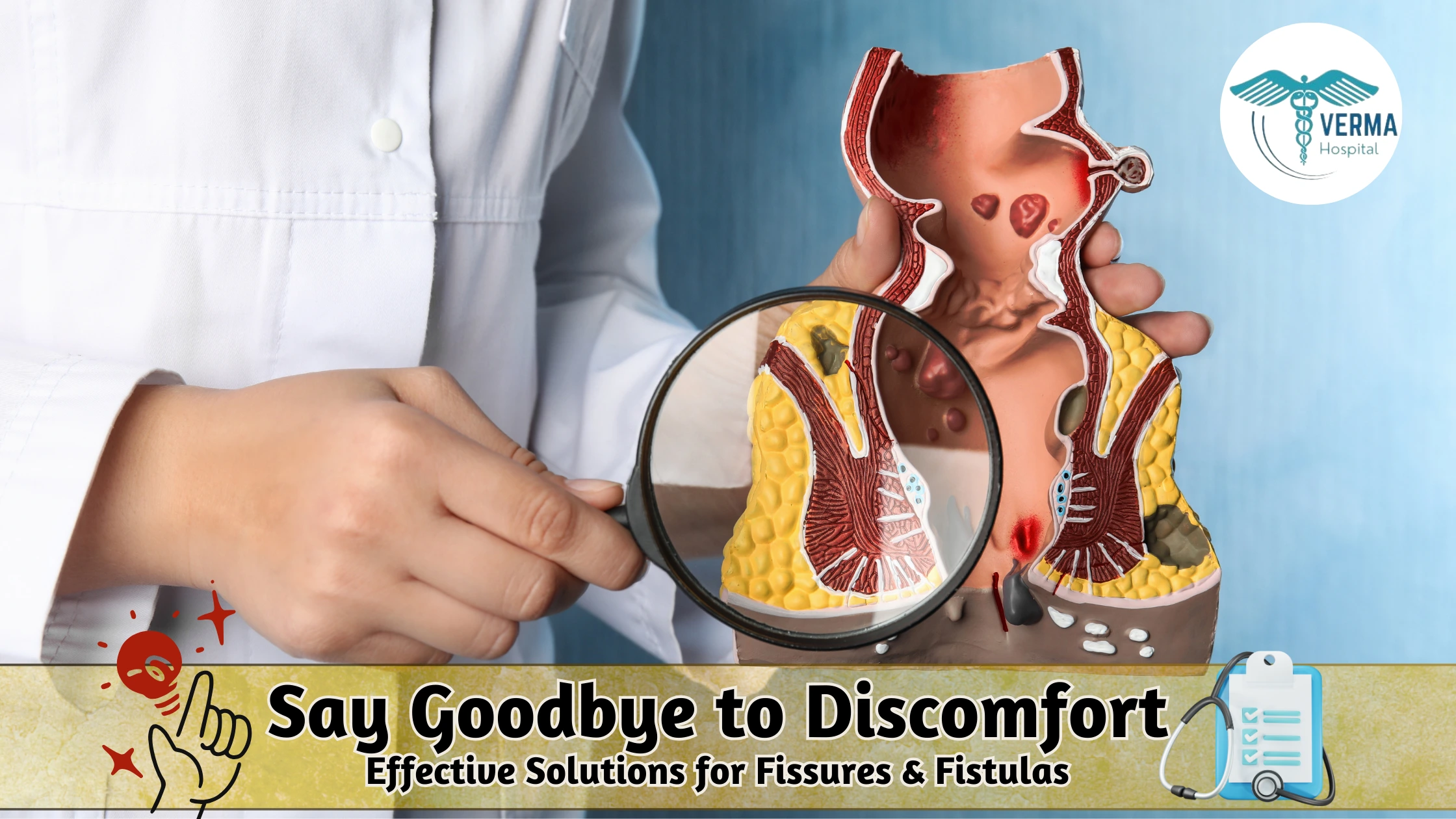
An anal fissure is a small tear in the lining of the anus, leading to pain and bleeding, especially during bowel movements. This condition can affect individuals of all ages but is most common among teenagers and middle-aged adults.
Types of Fissures
- Acute Anal Fissures: Caused by trauma or injury to the anal canal and may heal with conservative treatment.
- Chronic Anal Fissures: Last for more than six weeks and often require medical intervention.
- Primary Anal Fissures: Develop without any underlying medical conditions.
- Secondary Anal Fissures: Occur due to conditions like Crohn’s disease or HIV.
Causes of Fissures
- Reduced blood flow due to diabetes or cardiovascular diseases
- Low-fiber diet leading to constipation
- Passing hard stools or chronic diarrhea
- Inflammatory bowel diseases like Crohn’s disease
- Anal trauma from childbirth or medical procedures
Advanced Treatment for Anal Fissures
While home remedies, including dietary modifications and sitz baths, may help in mild cases, Laser Treatment for Anal Fissures in Mathura is a highly effective option for faster healing and minimal pain. This advanced technique ensures quicker recovery with fewer complications, making it a preferred choice for patients suffering from chronic anal fissures.
Consult an expert to determine the best course of treatment for long-term relief from anal fissures.
Fistula: Understanding the Causes, Symptoms, and Best Treatment
A fistula is an abnormal tunnel-like connection between two body parts that are not usually connected. This condition often results from infections, surgeries, or chronic inflammation. The most common type is an anal fistula, which forms between an anal gland and the skin around the anus, causing pain and discharge.
Types of Fistulas
- Anal Fistula: Forms due to infection and connects the anal gland to the skin around the anus.
- Intestinal Fistula: Develops between parts of the intestines or other organs, often post-surgery.
- Rectovaginal Fistula: Abnormal passage between the rectum and vagina, allowing stool leakage.
- Vesicovaginal Fistula: Forms between the bladder and vagina, leading to involuntary urine leakage.
Causes of Fistulas
- Chronic infections leading to abscess rupture
- Inflammatory bowel diseases like Crohn’s disease
- Surgical complications
- Trauma or injury to tissues
Best Treatment for Fistula
Fistulas often require surgical intervention to prevent infections and restore normal function. Laser Treatment for Fistula in Mathura is a cutting-edge procedure that offers precise healing with minimal discomfort and faster recovery. This treatment is highly effective in closing the abnormal passage while reducing the risk of recurrence.
If you suspect a fistula, consult a specialist for an accurate diagnosis and the most suitable treatment options.